Most people get this vaccine to avoid a painful
skin rash.
Nobody told them it might also protect their brain.
New research is revealing something extraordinary
about a shot millions of people already have access to —
and the implications for dementia prevention
could be enormous.
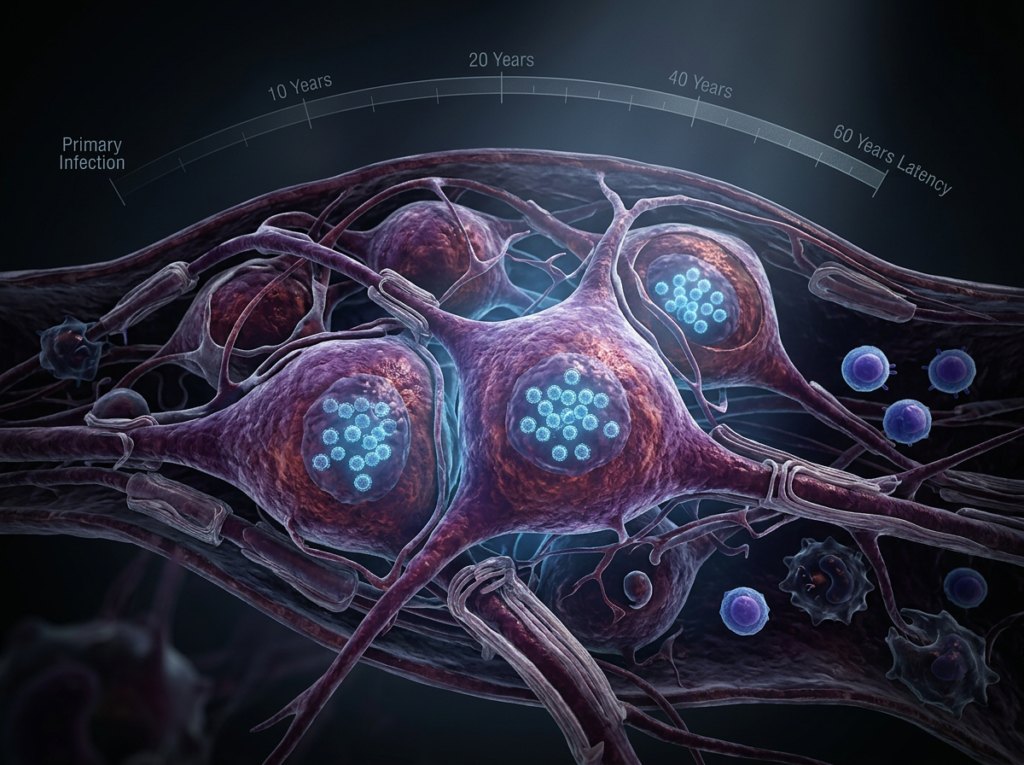
The Virus Hiding in Your Body Right Now
If you had chickenpox as a child,
the virus never left your body.
It retreated into your nervous system,
where it has been hiding ever since —
sometimes for 60 years or more.
Professor Cornelia van Duijn of Oxford University
explains: “The chickenpox virus can remain
latent in our bodies for over 60 years
since first exposure in childhood.”
Why can’t your immune system destroy it?
Because it hides inside nerve cells —
the most protected cells in your body.
Your immune system won’t attack them
for fear of causing damage.
So the virus waits. Patiently. For decades.
When It Wakes Up
As you age and your immune system weakens,
the virus reactivates.
It travels along nerve pathways,
causing the burning pain and blistering rash
known as shingles — one of the most
painful conditions a person can experience.
But the skin rash isn’t the real danger.
Every time the virus reactivates,
researchers believe it leaves microscopic
damage in the brain. Over time,
that damage accumulates.
Professor van Duijn puts it starkly:
“When the long-dormant virus reactivates,
it not only causes a very unpleasant skin condition
but may also be involved in dementia.”
Think of it as the virus delivering
a final knockout punch to a brain
that’s already under pressure.
The Shot That Changes Everything
There’s a vaccine for shingles.
Most people think of it as a skin disease prevention shot.
But a wave of new research suggests
it may be doing something far more significant —
protecting the brain itself.
The Wales Study:
In a large-scale study conducted in Wales,
people who received the shingles vaccine
had approximately 20% lower risk of dementia
compared to those who didn’t.
That’s not a small lifestyle difference.
That’s a statistically significant finding
that’s hard to explain away.
The U.S. Study (100 Million People):
An analysis of data from 100 million Americans
found that vaccinated individuals took
longer to receive a dementia diagnosis —
and the effect was strongest in those who
completed the full two-dose course.

Why Two Shots Matter
This is the critical detail most people miss.
One shot helps. Two shots is where
the real protection kicks in.
The logic is straightforward: the vaccine
prevents the virus from reactivating.
Every reactivation event potentially
damages the brain. Preventing reactivation
removes the opportunity for that damage entirely.
Two doses creates stronger, longer-lasting immunity —
meaning fewer reactivation events,
meaning less cumulative brain damage over time.
Who Should Get It?
Medical experts currently recommend:
- Adults 50 and older: 2 doses of shingles vaccine
- Adults 19 and older with weakened immune systems
or scheduled immunosuppressive treatment: 2 doses
If you’re in either category and haven’t
been vaccinated — this research suggests
it’s worth a serious conversation with your doctor.
The Bigger Picture
We don’t have a cure for dementia.
We don’t have a reliable way to prevent it.
But a vaccine that already exists,
is already approved, is already available —
and may reduce dementia risk by 20%?
That’s not nothing. That’s potentially one of
the most significant public health findings
in years.
Have you or a family member received the shingles vaccine? Will this research change your mind about getting it? Tell us in the comments. 👇